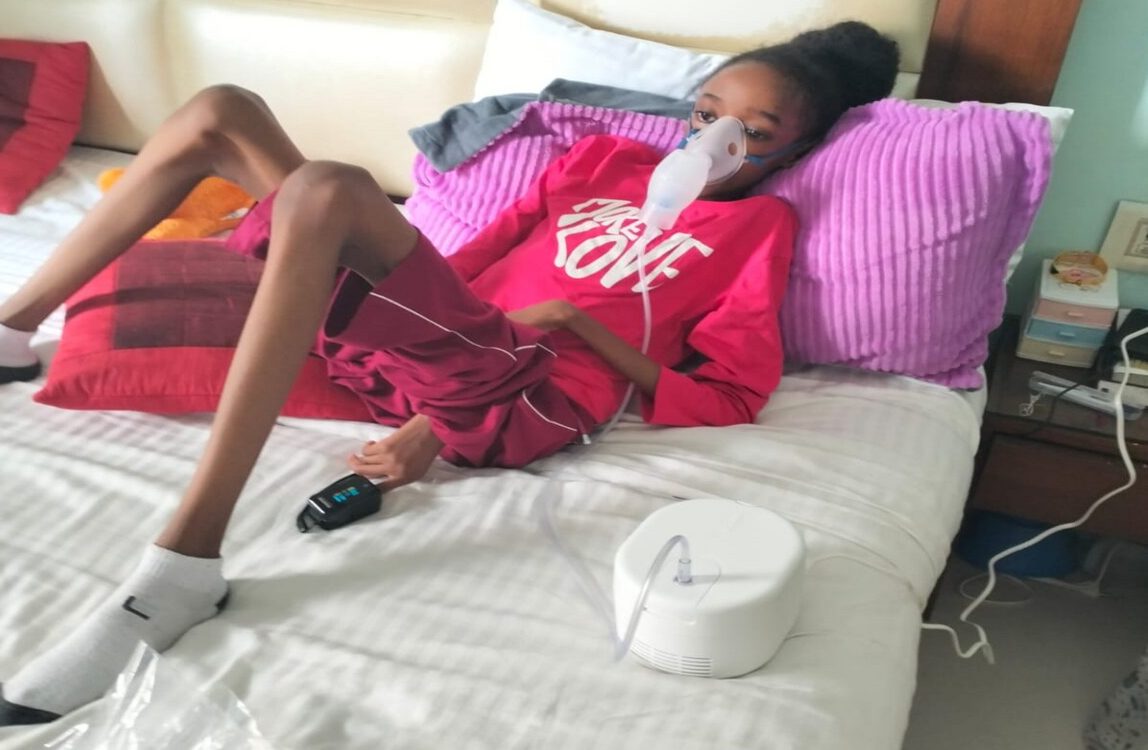
In 2023, Kenya’s Parliament dismantled the National Hospital Insurance Fund (NHIF) and ushered in the Social Health Authority (SHA), a bold restructuring aimed at universal health coverage. SHA was split into three pillars: Primary Health Care Fund; Emergency, Chronic, and Critical Illness Fund; Digital Health Authority
A mandatory 2.75% income deduction for salaried workers was introduced, sold as a transformative step toward equitable healthcare. The promise was grand promising accessible, comprehensive care for all Kenyans, from urban centers to remote villages.
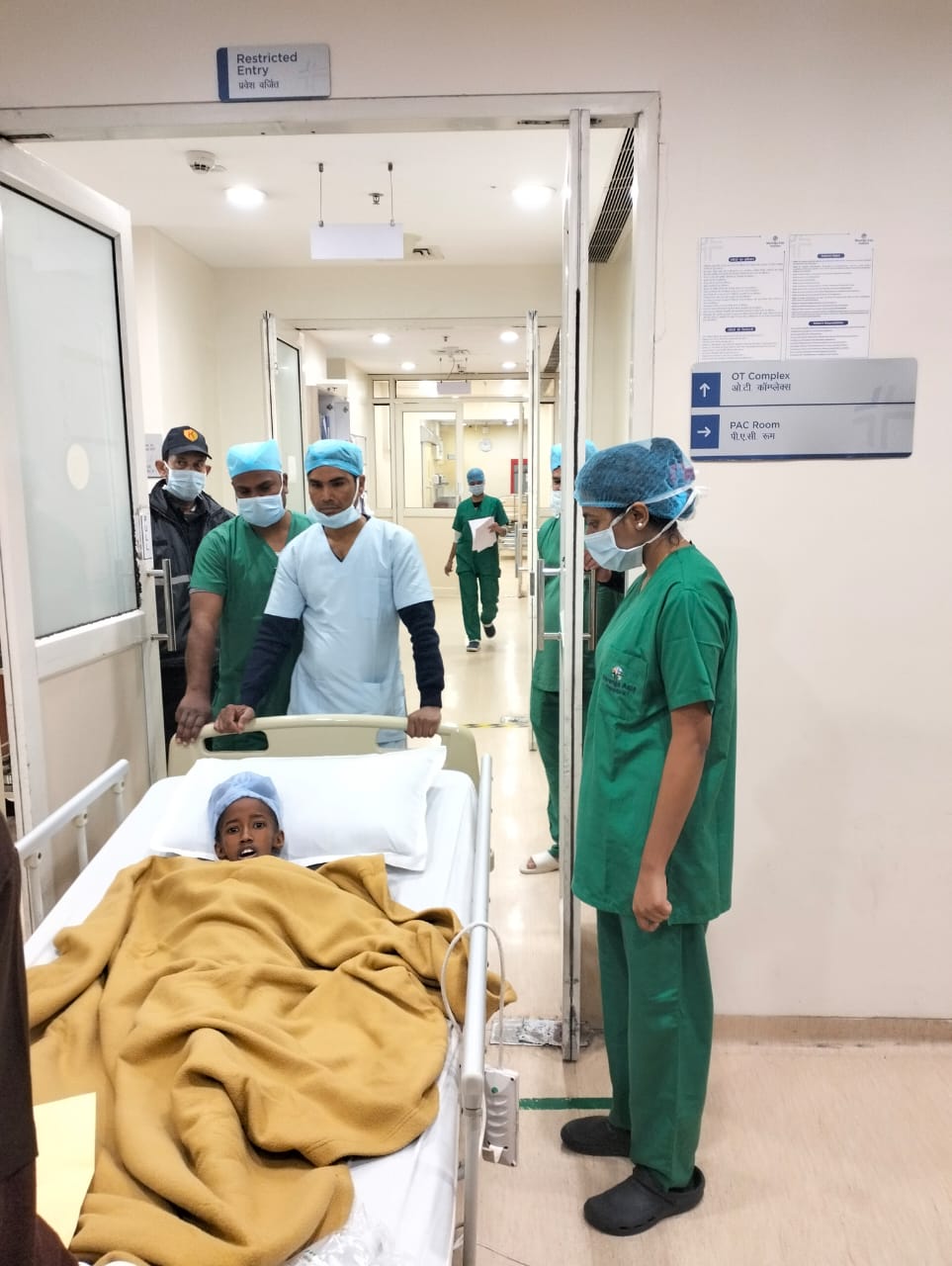
Yet, two years on, the sheen has faded into despair. Outpatient services that include basic clinic visits and diagnostic tests are excluded from SHA’s coverage, leaving families grappling with crippling out-of-pocket costs.
In 2023, the Parliamentary Budget Office flagged that Kenyans were already spending KES 150 billion annually from their pockets on healthcare.
A 2025 Kenya National Bureau of Statistics report reveals a 3.3% spike in costs, tightening the noose on households already stretched thin with high taxes, dwindling income generating opportunities and theft of public funds.
Economist Alexander Kireria, a veteran health policy analyst, calls the rising cost of healthcare a “systemic betrayal.”
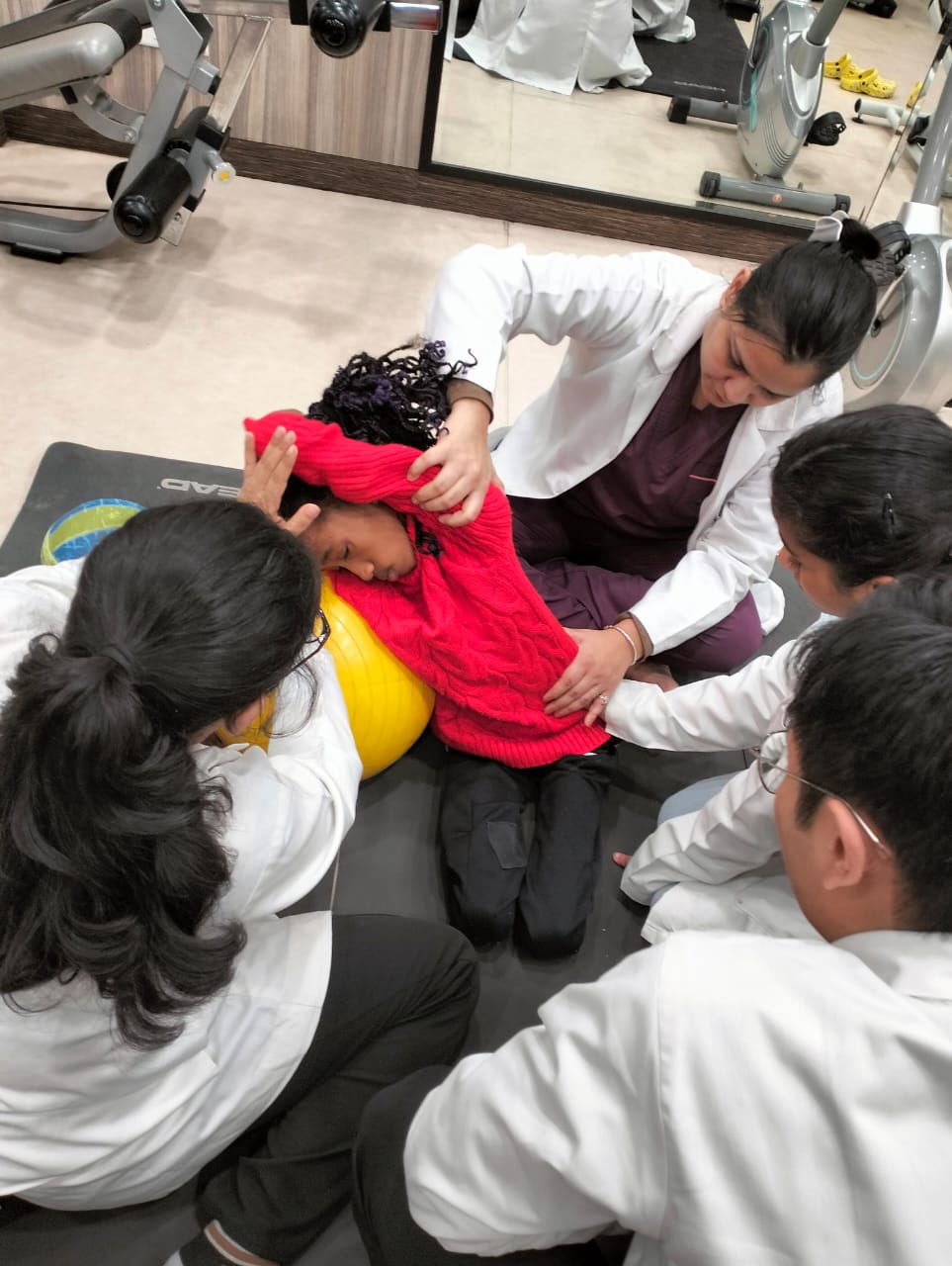
“In the past, the state financed up to 80% of healthcare expenses, easing the burden on households. This trend has however been reversed in recent years with households shouldering the burden,” he says.
With 40 years navigating Kenya’s health sector, including donor communities, Kireria has seen the system’s underbelly: fragmented funding, overstretched facilities, and unfulfilled promises.
“After the 2010 constitution, healthcare became devolved, a move meant to bring services closer to the people and address long-standing inequities. But counties are underfunded, stuck with wage bills and little left for services. Then households pay,” he asserts.
The NHIF’s was riddled with theft that left millions lost to corruption and a bloated system that failed the poor. SHA was meant to be a fresh start, a beacon of transparency. But experts like Kireria are warning that it is teetering on the same precipice.
“Without robust oversight, SHA risks repeating history. If the funds, the purchasing and the claims processing are not clean, the burden shifts back to the patient,” he says.
Tragically, those warnings have proven prophetic, as a massive scandal now engulfs SHA, exposing the depths of governmental rot.
Corruption’s deals deadly stranglehold on SHA
Just as SHA promised a new era, recent revelations have laid bare its descent into chaos. Rogue hospitals and “ghost facilities” have been used to siphon off billions from the system through fraudulent claims.
These scams targeted an astounding KES 10.6 billion, turning public health funds into private plunder while legitimate hospitals starve for payments.
Further, the Auditor General’s damning report exposed unbudgeted procurements for SHA’s systems, breaching laws through non-competitive processes that scream of insider deals.
Public outrage has mounted, with activists and politicians decrying the scandal as a “kleptocracy” where even the sick’s lives mean nothing.
President William Ruto has promised sweeping crackdowns, but critics dismiss the moves as too little, too late, more about damage control than genuine reform. There is also pessimism as Kenyans have come to be wary of most of their President’s promises. Many argue that Kenyans would only take him seriously if he went further and dismissed his health minister and senior officials, since ultimate accountability rests with them.
The SHA runaway corruption isn’t just theft, but a poverty trap. Millions of Kenyans, already burdened by the 2.75% deductions, now face a broken system where claims go unpaid, forcing hospitals to demand cash from desperate patients.
Legitimate providers teeter on collapse, while ghost entities feast, widening regional inequities and pushing families deeper into debt.
For cancer patients it’s race against time, money, and indifference
For Kenya’s cancer patients, SHA’s gaps, and now its scandals, are more than policy failures. They are a death sentence amplified by graft. The National Cancer Institute of Kenya reports 47,000 new cases annually, with 32,000 deaths, largely due to late diagnoses exacerbated by an unreliable, corruption-riddled national health system.
Phoebe Ongadi, Executive Director at Kenya Network of Cancer Organizations (KENCO), a patient-turned-advocate, says many families are driven into poverty within months of diagnosis.
“Cancer treatment is very expensive. SHA offers KES 400,000 per person, plus KES 150,000 from the Emergency, Chronic, and Critical Illness Fund. But this is considered a family payment. Under NHIF, spouses could pool for up to KES 1.2 million,” she says.
Now, with fraud draining funds, even these meager covers evaporate. Private hospitals, citing non-payments from SHA amid the scandal, demand out-of-pocket fees, creating a double burden.
“Hospitals tell us they are billing SHA, but the money is not coming. They can’t run on promises, so patients top up,” Phoebe explains.
Treatment abandonment skyrockets as families choose between treatment and food, all while corrupt officials siphon billions meant for life-saving care.
Capitation chaos adds insult: “Under NHIF, your year was clear. SHA’s financial year is a moving target – September, October? Cancer doesn’t wait,” says Phoebe. With ghost claims prioritized over real patients, tumors grow unchecked, and hope withers in a system where government indifference turns illness into destitution.
The vision of SHA was a lifeline for Kenya’s most vulnerable. But entangled in rampant corruption, an uncaring bureaucracy, and a broken framework, it has become a noose, condemning millions to poverty and preventable suffering in a health system beyond redemption.
By Eunice Omollo